-
(a) What is the most likely diagnosis and what is your differential diagnosis?
Show Answer
The most likely diagnosis is recurrent small pulmonary emboli as this patient is at high risk due to immobility and the need for a plaster cast, lower limb trauma with potential vascular damage and the clinical history of recurrent short-lived episodes of hypotension. Although less likely, chest infection, arrhythmias and ischaemic heart disease are other possibilities that should be considered.
-
(b) Which investigations will you perform, and in what order, to confirm your diagnosis and why?
Show Answer
Arterial blood gas abnormalities are common following a pulmonary embolus, including hypoxaemia with a widening of the alveolar–arterial (A–a) gradient, hypoxaemia and hypocapnia (despite increased dead space). In the majority of patients the ECG is not helpful and shows non-specific ST segment changes. However, about one-third of patients with large pulmonary emboli develop a right ventricular strain pattern with the classic changes of an S wave in lead I and a Q wave and T wave inversion in lead III (S1Q3T3 pattern), right axis deviation and right bundle branch block. Most patients have non-specific abnormalities on chest X-ray including atelectasis due to reduced surfactant production in areas of poorly perfused lung. The presence of a lower limb deep venous thrombosis (DVT) should be sought with a Doppler ultrasound scan (or impedance plethysmography). Echocardiography may show right ventricular dysfunction and pulmonary hypertension. A transoesophageal echocardiograph may detect emboli in the main pulmonary arteries but not in lobar or segmental arteries.
A ventilation/perfusion (V/Q) scan is usually the initial diagnostic investigation. A negative perfusion scan rules out a pulmonary embolus, whereas a ‘high-probability’ scan (i.e. multiple segmental perfusion defects and associated normal ventilation) has a >85% probability of a pulmonary embolus. With a high clinical suspicion, a high-probability V/Q scan has a positive predictive value >95%. Unfortunately, most V/Q scans are not diagnostic or are indeterminate with a 15–50% likelihood of pulmonary embolism, necessitating further imaging. Absence of a DVT combined with a low-probability V/Q scan permits withholding treatment, whereas a negative Doppler ultrasound scan with an intermediateprobability V/Q scan (or underlying cardiac or pulmonary disease) necessitates further imaging. Spiral CT scans have a sensitivity for pulmonary embolus of 70–95% (higher for more proximal emboli) and a specificity >90%. CT also allows visualization of parenchymal abnormalities and is useful in patients with COPD or extensive chest X-ray abnormalities where V/Q scanning is indeterminate. Magnetic resonance imaging (MRI) scans are more specific and sensitive but not widely available. Pulmonary angiography remains the diagnostic standard but is invasive.
-
(c) In what other ways can this condition present?
Show Answer
Patients with pulmonary embolism present with pleuritic pain and haemoptysis in about 65% of cases, isolated dyspnoea occurs in about 25% and circulatory collapse in about 10% of cases. Dyspnoea is not present in about 30% of patients with confirmed pulmonary embolism. Other non-specific features include apprehension, tachypnoea, tachycardia, cough, sweating and syncope. Following a large pulmonary embolus features of right ventricular failure (e.g. hypotension, jugular venous distension) may occur.
-
(d) What immediate treatment would you recommend?
Show Answer
Anticoagulation stops propagation of existing lower limb thrombus and allows organization of the remaining clot, which reduces the risk of further emboli. Immediate therapy in patients with a high suspicion of a pulmonary embolus may prevent further life-threatening emboli. Unfractionated heparin (UH) or low molecular weight heparin (LMWH) for 5–7 days, is followed by warfarin for 4–6 weeks when temporary risk factors (as in this case) are the cause and for 3–6 months in idiopathic cases. UH and warfarin must be monitored, as subtherapeutic levels increase the risk of recurrent thromboembolism. LMWH is more bioavailable and does not require monitoring. About 20% of patients with thromboembolic disease have inherited or acquired hypercoagulation problems (e.g. antithrombin III deficiency, protein C deficiency, lupus anticoagulant) and may require lifelong therapy. If contraindications prevent anticoagulation (e.g. recent surgery, haemorrhagic stroke, CNS metastases, active bleeding) or emboli occur while on therapeutic anticoagulation, an inferior vena cava filter may prevent further pulmonary embolism.
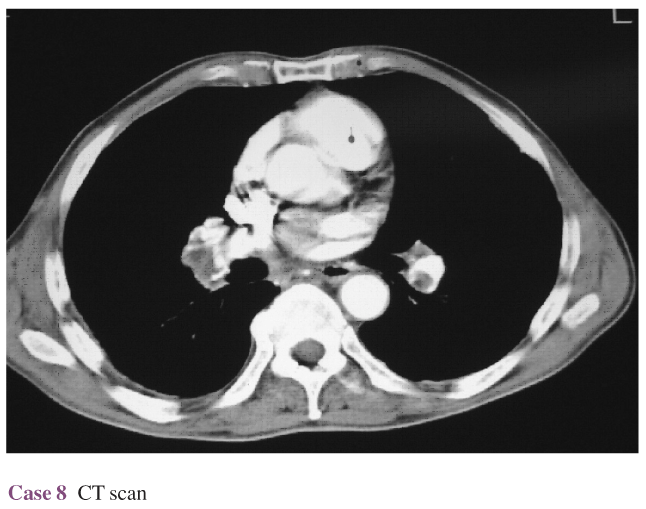
- Later the same day, following return from further investigations in the radiology department, the patient reports a sudden onset of severe breathlessness. He rapidly becomes cyanosed with a saturation of 65%. You are on the ward and have been able to briefly assess the patient. He is cold, clammy, cyanosed and confused, with a thready pulse, low blood pressure and raised jugular venous pressure. The CT scan images are available but have not been reported (Fig. Case 8). The oxygen flow has been increased to maximum and you have inserted a venous catheter when the patient suddenly arrests.
-
(e) What is the likely cause of the arrest and what immediate management would you institute while awaiting the arrest team?
Show Answer
The CT scan in Figure Case 8 confirms the presence of pulmonary emboli in both pulmonary arteries. A single, sudden, large embolus with marked obstruction of pulmonary blood flow is the likely cause of the cardiac arrest. In general, circulatory collapse occurs with >50% obstruction of the pulmonary arterial bed. Smaller emboli may be fatal when pre-existing lung or heart disease coexist. Cardiopulmonary resuscitation must be started immediately. The cardiac massage may help break up a large clot into smaller segments which travel distally and reduce the degree of pulmonary bed occlusion. Following intubation high-dose oxygen must be administered. Immediate plasma expanders and inotropic support are often given in an attempt to increase right ventricular pressure and to displace clot distally, but risks of right ventricular distension and subsequent myocardial damage are severe.
-
(f) Would you consider thrombolytic therapy in this patient?
Show Answer
Thrombolytic therapy is recommended in severe life-threatening massive pulmonary embolism with cardiovascular collapse. Thrombolytics hasten resolution of perfusion defects and correct right ventricular dysfunction, but there is limited evidence of survival benefit. Nevertheless, they would have been appropriate in this patient with life-threatening cardiovascular collapse. In patients without massive pulmonary embolism there is no survival benefit with thrombolysis and there is a substantial increase in bleeding complications, including a 0.3–1.5% risk of intracerebral haemorrhage. Consequently, thrombolysis is not recommended in these patients.